Did you know acupuncture could improve endometrial lining and embryo implantation? In this recent study (2019) acupuncture increased pregnancy rates by 13% and the effect of estrogen therapy on endometrial lining. The endometrium was thicker after acupuncture and it improved the type of linings to those associated with good receptivity and higher implantation rates (tri-layer, type A). Acupuncture increased blood flow to the uterus by reducing resistance in the uterine arteries.
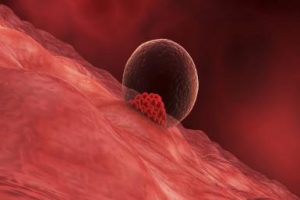
Acupuncture improves endometrial thickness & pregnancy rates